Headaches are a complicated subject because there are many different headache types and there are often many factors involved in their development (often, there is not one single identifiable cause). This article serves as an introduction to the topic of headaches with some tips about management and prevention. More information about headache classification can be found on the International Headache Society website.
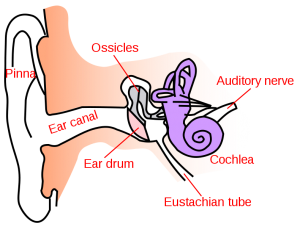
The most common type of headache, responsible for ~90% of all headaches, is a tension type headache (TTH). Pain quality is described as a tensor band squeezing the head, bilateral across the temples and/or around the base of the skull. TTHs, along with a few other headache types have musculoskeletal components to their etiology. For example, tight muscles in the neck and shoulders and the joints of the neck and jaw can refer pain to the head. Overall posture and especially head carriage can be responsible for the development of joint irritation and muscle tension that results in headache development.
Management and Prevention Tips:
-
Have a proper evaluation:
Most headaches are benign in origin but having a proper diagnosis is important because the management may differ. In addition, certain “red flags” may indicate a pathology that must be taken seriously. Make sure to consult with a healthcare professional if the headache is severe, different from your typical headache has an abrupt onset or is associated with trauma, neurological signs, fever, other unusual symptoms or if you have concerns.
-
Create a headache diary:
If you have headaches frequently, creating a headache diary may be beneficial. This will help identify your possible triggers such that you can avoid them. Jot down what you were doing, eating, drinking, feeling, the type of environment you were in, the quality of your sleep, and amount of stress you felt during the 24 hours prior to headache onset. When you see a health professional about your headaches, you can also discuss your headache diary.
-
Avoid headache triggers:
Once you establish your headache triggers, you can try avoiding them. Some common triggers are food sensitivity / allergy, coffee, alcohol, stress, dehydration, loud sounds, bright lights, hunger and poor sleep. Wear sunglasses if bright light triggers your headache.
-
Improve your posture:
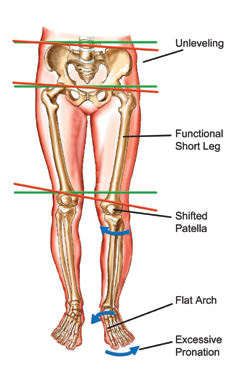
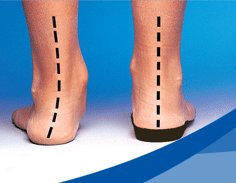
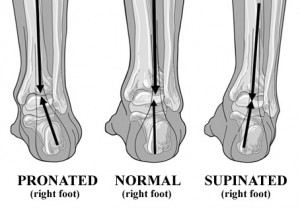
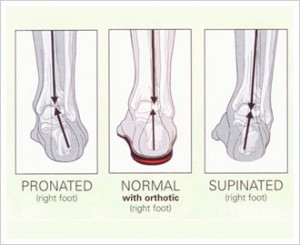
Headaches are often associated with posture – especially head carriage. Having optimal posture reduces the stress on muscles, joints and ligaments that can otherwise refer pain to the head resulting in a headache. The biggest culprit is the forward head carriage where the chin and head jut forward relative to the shoulders. The muscles of the neck must work harder and tense to counterbalance the weight of the head (which is like a bowling ball sitting on your neck). Forward head carriage is common in students and office workers who slump forward at a computer for hours each day. Loss of the normal curve of the neck may also be associated with headaches due to joint irritation. A chiropractor can provide you with specific exercises for improving posture and advice regarding office ergonomics.
-
Exercise regularly:
Regular cardiovascular exercise is good for overall health and stress relief.
-
Stop smoking:
Smoke may be an allergen that triggers headaches. In addition, nicotine has an effect on the vascular system and the vascular system is thought to trigger certain types of headaches – especially migraines.
-
Reduce stress:
Overall stress reduction may help headache sufferers. Take some time to enjoy hobbies, socialize and exercise so that there is balance between work and play. Some stress relieving activities include yoga, thai chi and meditation.
-
Regular sleep pattern:
Getting enough sleep is just as important as maintaining a regular sleep-wake cycle. There are natural fluctuations in the body – for hormone levels, sugar levels and enzyme levels – which are influenced by sleep-wake cycle. These are know as circadian rhythms. Disruption of circadian rhythms may be responsible for headaches in some people. As far as quantity of sleep goes, the typical recommendation is 8 hrs of uninterrupted sleep per night. The best sleep positions for the back and neck are on your back or side (never sleep on your stomach).
-
Find a cool dark place to nap:
Sometimes when a headache hits, the best thing to do is to lay down and let the headache run its course.
-
Apply cold or heat
Applying a cool, moist cloth across the forehead or base of the skull can be especially good for relieving headache pain.
-
Visit your chiropractor:
As previously mentioned, headaches are often associated with tight muscles and dysfunction of joints of the neck or jaw. Regular spinal check-ups and adjustments as part of a wellness plan help keep headaches at bay in many people. Chiropractors are also trained to identify red flags associated with headaches and to refer accordingly if necessary.
-
Other:
Other natural methods for headache relief include acupuncture and massage therapy.
Headaches can be significantly disruptive to everyday life. I hope these tips have been helpful.